Often, public attention gravitates to simple fixes to large-scale problems — with reason, as such solutions are appealing, and sometimes they work. But a recent flurry of projects is supporting health through complex packages of solutions, including an organization supporting vision in Africa, a tech project in South Asia and even part of America’s Affordable Care Act.
In global health and development, is complexity the new simplicity?
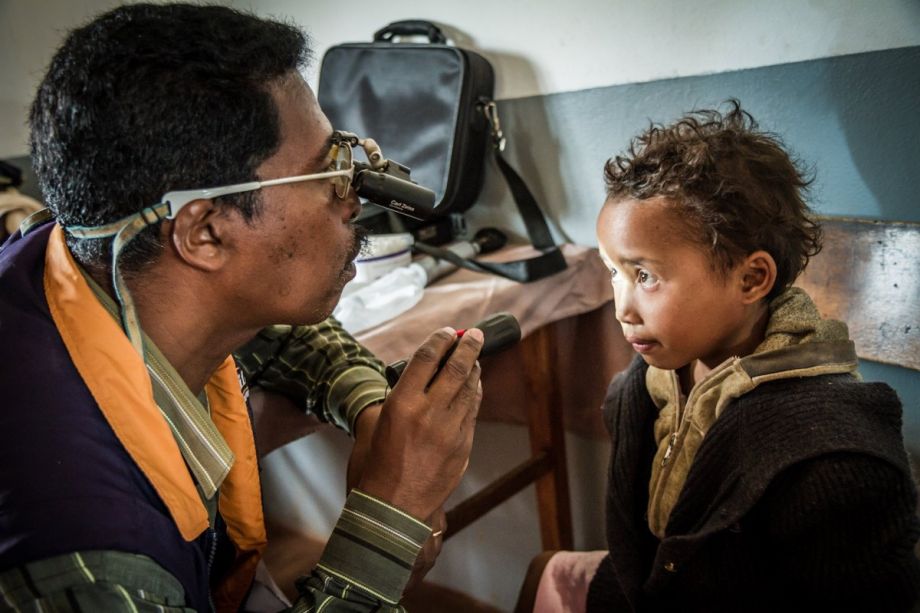
Paul Courtright thinks it is. He’s one of the founders of the Kilimanjaro Centre for Community Ophthalmology, a project that just won the prestigious Antonio Champalimaud Vision Award for innovations in eye care. Since 2001, he and his collaborators have been expanding the capacity of healthcare facilities in sub-Saharan Africa to address patients’ visual health.
The help is sorely needed. Like people everywhere, Africans often experience worsening vision with age. Along with this issue comes a range of visual disorders in excess of the ones that trouble Western people: loss of vision from undiagnosed diabetes, for instance, and trachoma, an infectious disease that causes the eyelids to turn inward and blind the eye. (The latter has been eradicated in most countries outside of sub-Saharan Africa.) As is the case with most healthcare specialties, Africa has far fewer providers than are necessary to treat all people who need care.
KCCO (and the partners with whom it shared the prize, the Seva Foundation and Seva Canada) isn’t alone in attempting a fix for the problem. But their approach differs from the simple fixes — like adjustable glasses or a smartphone-mounted eye-testing device — that global health projects sometimes offer. While those can generate a positive impact, KCCO’s collaborative Kilimanjaro Project instead provides a multipronged program that aims at increasing care by increasing the capacity of existing African clinics.
“We don’t provide clinical care,” Courtright says. Instead, the project encompasses research, training, technical advice and evaluations meant to help existing healthcare facilities provide better eye care to their patients. The project’s wraparound approach can allow a neat complement to simpler innovations, as it can theoretically move useful tech solutions to the right place and right population at the right time.
“We do look at it as a comprehensive model,” Courtright says.
KCCO’s approach to providing care might be unique among sub-Saharan African visual health projects, but it is not unique in healthcare worldwide. In America, for instance, the changes triggered by the passage of the Affordable Care Act included a massive gamble on a concept called “care coordination.”
The method, invented by Sri Lankan-American physician Rushika Fernandopulle, aims to reduce healthcare spending by better managing chronically ill patients with high costs. To address the complexities these patients experience — often a mix of long-standing disease, acute social stresses and difficulty navigating an inefficient healthcare system — Fernandopulle constructed a team of dedicated practitioners to collaborate with each patient. These providers, termed “care coordinators,” try to remove every hurdle blocking a patient’s best health outcomes. The end result is often healthier, happier patients and lower expenditures. (Disclosure: In the past, I’ve worked on care coordination projects for Illinois Medicaid.)
Care coordination, like the KCCO model, is simple only in that it unites a huge and varying array of problems under one large umbrella. The model is out of step with the trending, simple tech approach to solutions, like a $100 laptop held up as the answer to an insufficient education for millions of children. Courtright says, “People want to hear simple stories,” and notes that it’s sometimes been a block to KCCO’s development.
Yet, as KCCO’s prestigious award suggests, complexity might be the new global vogue. Earlier this year, former Microsoft programmer Kentaro Toyama published Geek Heresy, a kind of confessional-cum-manifesto about technological solutions to global problems. Identifying himself as a “technology addict in recovery,” Toyama builds his conclusions around the five years he spent researching and implementing technological innovations for global development in India.
The book doesn’t discount the value of simple fixes, some of which are undeniable (many people in Kibera, a slum in Nairobi, Kenya, for example, wouldn’t mind having a smartphone and an emergency number to call). But, using an example of an organization called Digital Green that worked by combining new technology with high-touch, person-to-person communication, Geek Heresy agitates against believing overly simplistic, one-note fixes — what Toyama calls “packaged interventions” — are enough.
“What isn’t a packaged intervention?” he writes. “The caring attention of a good teacher. Citizen participation in a protest march. The capable execution of a vaccination program by a well-managed healthcare system ….” Even the best technological solutions, he concludes, must be implemented by embracing “the importance of heart, mind, and will.”
Courtright agrees. “Unless you have good leadership or the potential for good leadership and team management in place, you can throw in all kinds of money and not get much out of it,” he says. By promoting human wisdom and connection, “We help places become productive and to expand their service selections.”
The Champalimaud Award committee believes in the value of the approach. But does a person in need agree?
At least one does. I met 34-year-old Michael Kazala on a street corner in downtown Nairobi, where he was sitting on an upturned bucket and cradling a guitar. With his head tilted towards his instrument, it was hard to see his face. But when he looked up, his eyes – one socket empty, and the other bearing a cataract-blinded, rolling eyeball – were striking.
“I lost my sight from the measles,” at age 10, he said. Bright, upbeat and not lacking in ambition — he’d like to tour the U.S., he said, playing clubs — Kazala was nonetheless badly hobbled by the aftereffects of a disease that could have been prevented with a cheap, simple technology: a vaccine.
Only complexity would make up for its absence. Living in the street, he relied on the sole job he could do, blues busking. He could readily list the help he needed, including comprehensive medical care, disability assistance and support in securing housing. But he said the healthcare system continued to offer him little.
What he was describing seemed to encompass both simple technologies and the wise implementation of them; the back-on-your-feet effort of care coordination; and the comprehensive approach to visual health that the Kilimanjaro Project helps primary care clinics provide. “Everything,” Kazala said, summarizing his needs in the simplest possible terms.
Smiling into the twilight he could not see, he said it once more for emphasis: “Everything.”
The “Health Horizons: Innovation and the Informal Economy” column is made possible with the support of the Rockefeller Foundation.

M. Sophia Newman is a freelance writer and an editor with a substantial background in global health and health research. She wrote Next City's Health Horizons column from 2015 to 2016 and has reported from Bangladesh, India, Nepal, Kenya, Ghana, South Africa, and the United States on a wide range of topics. See more at msophianewman.com.
Follow M. Sophia .(JavaScript must be enabled to view this email address)